How the Precise Behavioral digital platform helps clinicians coordinate care, monitor PHQ-9 and GAD-7 scores, and support families between appointments.
Written by Emily Yi, LCSW, a Licensed Clinical Social Worker (LCSW) and Clinical App Monitor at Precise Behavioral.
One of the most critical gaps in adolescent mental health care occurs the moment after a therapy session ends.
A parent may leave the office worried about their teen’s depression. A teenager may still be processing difficult emotions that surfaced during the conversation. As clinicians, we often wish for the ability to provide families with more support in those moments by offering something immediate, reliable, and clinically grounded.
At Precise Behavioral, our digital behavioral health tools offer the opportunity to extend clinical care beyond the therapy session by providing evidence-based psychoeducation, symptom monitoring, and coordinated follow-up.
This case study highlights how the Precise Behavioral digital platform supported collaboration among a therapist, a psychiatric provider, and a primary care physician, while also giving a teen patient access to trusted mental health resources and structured symptom monitoring between visits.
Background: Supporting Teens and Families Between Sessions
In my work with adolescents experiencing anxiety or depression, I often see the need my clients have for support that continues beyond the therapy session. However, our traditional care models typically rely on periodic appointments, leaving families with limited guidance between visits.
Parents frequently tell me that this is one of the most difficult parts of the process. When symptoms change or emotions arise unexpectedly, they are often unsure how to best respond or support their teen in the moment. The parents want to help, but often do not feel confident about what support is most effective.
From the clinical side, I also recognize the limitations of relying largely on patient recall to understand what has happened between sessions. Important symptom changes, functional decline, or warning signs can be missed when we are reconstructing events days or weeks later. This can delay intervention and make it more difficult to identify emerging concerns before they escalate.
This is where digital behavioral health tools can help address this gap. By providing structured monitoring, trusted psychoeducation, and accessible support resources, we support both patients and providers, offering continuous guidance and earlier visibility into changes over time.
Care Model: Collaborative Support for Teens
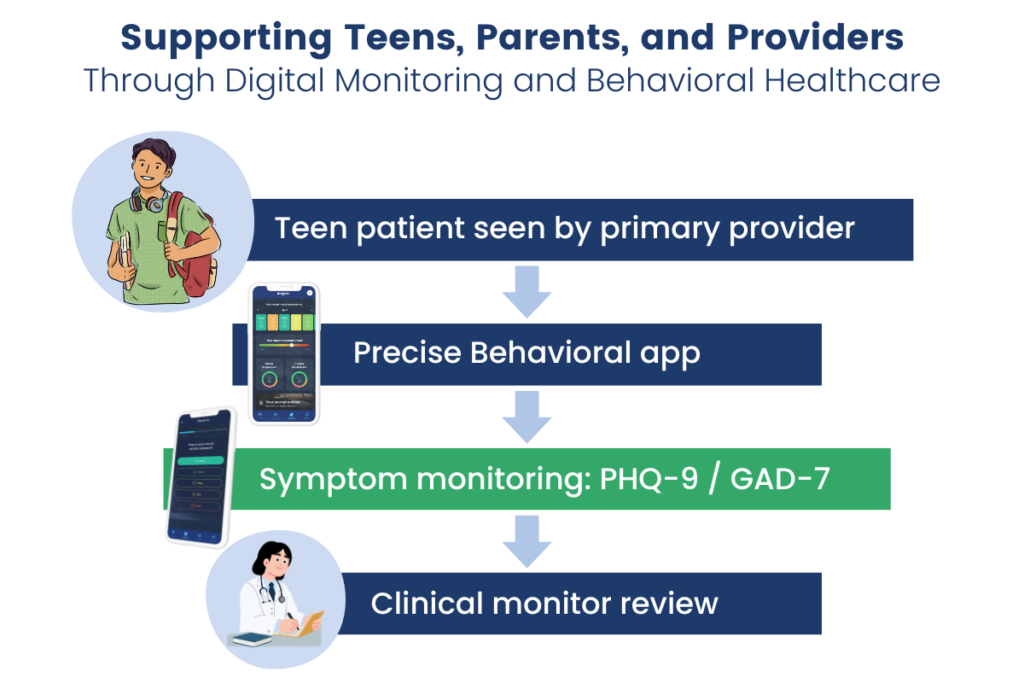
My role: Clinical App Monitor (Coordinator Role)
I served as the clinical app monitor, reviewing patient symptom data collected through the Precise Behavioral platform, including PHQ-9 and GAD-7 trends, engagement patterns, and AI-informed clinical alerts. In this role, I monitored for changes that suggested worsening symptoms, elevated risk, or the need for timely follow-up, and communicated concerns to the treatment team as needed.
Treating Clinician (Primary Care Physician)
The treating clinician (in this case, it was the client’s primary care physician) worked directly with the teen and their parents during therapy sessions, addressing emotional regulation, anxiety, and mood symptoms.
Psychiatric Provider at Precise Behavioral
A psychiatric nurse practitioner within the Precise Behavioral care team was available to provide consultation on medication management, symptom escalation, and treatment recommendations when symptoms indicated a need for additional support.
This collaborative approach helped ensure that both the patient and the provider were supported between sessions.
Immediate Support for Families After Sessions
One of the most common challenges I encounter as a clinician is how to support families in the time immediately following a therapy appointment.
Parents may leave the session with concerns about their teen’s well-being, while teens may still be processing difficult emotions discussed during treatment.
In this case, the Primary Care Physician (PCP) was able to offer the family immediate access to the Precise Behavioral platform, which provided:
- psychoeducational articles explaining anxiety and depression
- guided exercises based on cognitive behavioral therapy principles
- mood and sleep tracking tools
- structured symptom assessments, such as the PHQ-9 and GAD-7
Providing these resources allowed the PCP to offer the family practical support right away, rather than asking them to wait until the next scheduled appointment.
From a parent’s perspective, this often provides an immediate sense of reassurance. Families have shared that it feels grounding to know that their teen had access to reliable mental health information and evidence-based tools, rather than relying on potentially inaccurate content found on the internet or on social media.
Helping Teens Access Accurate Mental Health Information
A growing number of adolescents turn to online platforms for mental health information and support; however, the accuracy, reliability, and evidence base of content shared on social media vary significantly, ranging from clinically sound guidance to unverified or potentially misleading advice.
Through our Precise Behavioral platform, the teen had access to clinically informed psychoeducational content, including:
- explanations of anxiety and depression symptoms
- strategies for managing stress and emotional overwhelm
- guidance on sleep and emotional regulation
- cognitive behavioral exercises designed to help teens identify thinking patterns
Providing reliable information helped the patient better understand their experiences and offered structured strategies to use between therapy sessions.
Monitoring Symptoms and Preventing Patients from Falling Through the Cracks
Structured symptom monitoring is a core component of our platform, providing continuous, data-driven insight into patient health trajectories over time.
The patient regularly completed standardized assessments including:
- PHQ-9 (Patient Health Questionnaire) for depression
- GAD-7 (Generalized Anxiety Disorder scale) for anxiety
As the app monitor, I reviewed these scores to identify patterns that might indicate worsening symptoms.
In this case, the system allowed us to detect when the patient’s scores remained consistently elevated across multiple assessments, indicating the need for additional clinical attention.
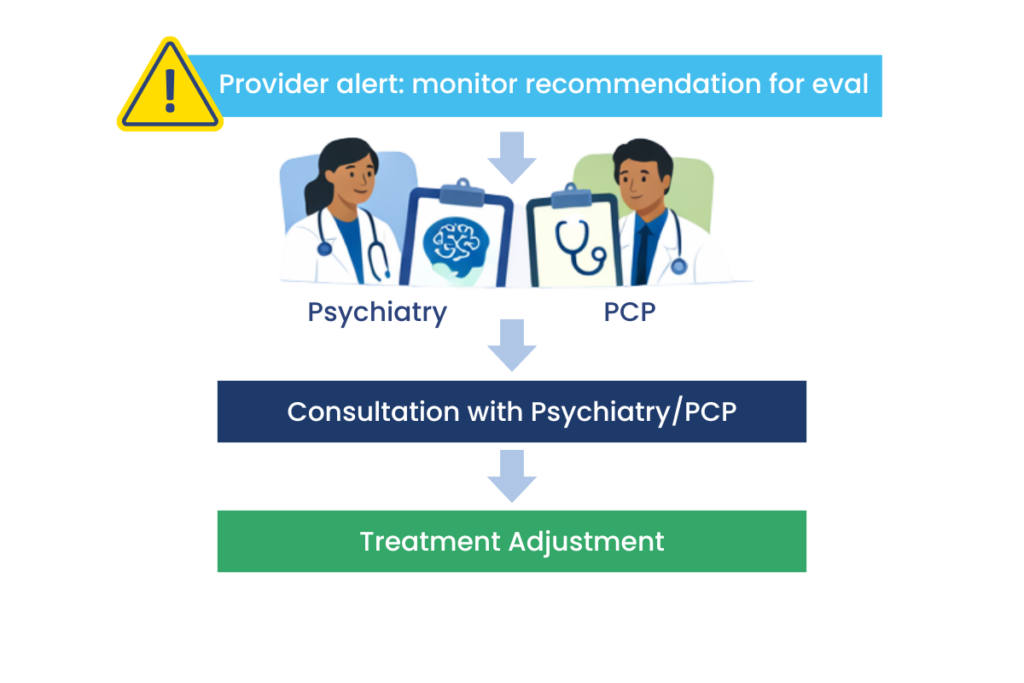
When these patterns emerged, I alerted the PCP and coordinated a consultation with the psychiatric provider.
This process helped ensure that the patient did not fall through the cracks between appointments and reduce the risk of missed symptom escalation, which can occur in traditional care models when symptom monitoring relies solely on patient recall.
Supporting Providers in Clinical Decision-Making
For all clinicians involved in treating the patient, I found the platform provided valuable support by offering us:
- real-time symptom data
- structured assessment results
- trends in mood, sleep, and anxiety levels
This information helped me and the rest of the care team better understand how the patient was functioning outside of the therapy session, in their day-to-day life.
When consultation was needed, I was able to review the patient’s symptom trends alongside the treating clinician and psychiatric provider, which allowed us to make more informed and timely treatment decisions.
Having these systems in place strengthened continuity of care and reduced the likelihood that important symptom changes would be missed between appointments.
The platform provided me as the monitor and coordinator confidence in supporting both the providers and the family, knowing the ongoing symptom monitoring, follow-up workflows, and care coordination processes were actively in place.
Operational Impact
While this case highlights our experience of a team of a monitor, psychiatric provider and primary care provider coordinating to help patients in the primary care setting, it also illustrates how digital behavioral health tools can support broader improvements in clinical workflow and care coordination.
Supporting Providers in Real Time
Mental health clinicians often carry significant responsibility for monitoring patient safety between appointments, yet traditional care models provide limited visibility into how patients are functioning day to day.
By incorporating structured symptom monitoring through tools such as the PHQ-9 and GAD-7, the Precise Behavioral platform provides clinicians with additional awareness of symptom trends between visits. Alerts triggered by sustained high scores allow providers to respond sooner when patients may need additional support.
This system helps clinicians feel more supported in their role, knowing that patterns indicating increased risk will not go unnoticed.
Strengthening Support for Families
For parents of teens receiving behavioral health care, the time between therapy sessions can feel uncertain. Families may be unsure how to respond when symptoms worsen or when difficult emotions arise.
The platform allows clinicians to offer families immediate access to trusted psychoeducational resources and structured exercises, helping parents and teens engage with evidence-based strategies, rather than scouring the internet and finding potentially inaccurate information.
Providing these tools immediately after sessions helps extend therapeutic support beyond the clinic.
Enabling Collaborative Care Models
The Precise Behavioral platform also creates a shared point of information for providers working across disciplines.
Primary care clinicians can collect structured behavioral health data from patients and use that information when consulting with psychiatric specialists. This approach supports Behavioral Health Integration (BHI) and Collaborative Care Model (CoCM) workflows, in which primary care providers work with behavioral health consultants to guide treatment decisions.
Digital monitoring tools can make these consultations more effective by providing objective symptom data rather than relying solely on retrospective patient reports.
Reducing the Risk of Patients Falling Through the Cracks
One of the most significant challenges in behavioral health care is ensuring that patients experiencing worsening symptoms are identified before a crisis occurs.
By combining regular symptom assessments, patient engagement tools, and provider alerts, digital platforms can help reduce the likelihood that patients with persistently elevated depression or anxiety scores go unnoticed between appointments.
This type of monitoring creates an additional layer of safety within the care system, while preserving the central role of clinicians in treatment planning.
Outcomes
The collaborative model supported several important outcomes:
Increased Provider Confidence
The primary care provider had greater confidence that the patient was being monitored between sessions, and that elevated symptom scores would trigger follow-up.
Immediate Resources for Families
Parents were able to leave therapy sessions with access to structured resources and guidance, reducing uncertainty between appointments.
Reliable Mental Health Information for Teens
The patient had access to evidence-based psychoeducation instead of relying on potentially unreliable online information.
Early Identification of Symptom Trends
Through regular monitoring of PHQ-9 and GAD-7 scores, I was able to identify sustained elevations and symptom trends early, allowing the care team to respond with timely consultation, follow-up, and treatment adjustments.
Implications for Behavioral Health Care
This case illustrates how digital behavioral health tools can support clinicians and families by extending care beyond the therapy session.
Key benefits include:
- providing teens with credible mental health information
- supporting parents between appointments
- helping clinicians monitor symptoms more consistently
- reducing the risk that patients experiencing worsening symptoms go unnoticed
When combined with interdisciplinary collaboration between therapists, psychiatric providers, and primary care clinicians, digital tools can strengthen the overall behavioral health care system.
The Future of Adolescent Behavioral Health Care
Adolescent mental health care increasingly requires collaboration across disciplines, including therapists, psychiatric providers, and primary care clinicians, to ensure comprehensive assessment, coordinated treatment planning, and continuity of care across both physical and psychological health needs.
Digital behavioral health platforms can help support this collaboration by providing structured symptom monitoring, reliable psychoeducation, and coordinated communication between providers.
In this case, the Precise Behavioral platform extended care beyond the therapy session by providing families with immediate resources while enabling clinicians to monitor symptom trends and coordinate timely follow-up when needed.
As healthcare systems continue to adopt integrated behavioral health models, digital tools may play a key role in supporting more consistent clinical care and reducing gaps in follow-up and patient support.
This case study describes a de-identified clinical scenario based on real-world workflows. All patient details have been modified to protect privacy.
Developed within this context, Precise Clinical brings these elements together through hybrid delivery, continuity-focused design, workforce-aware structures, and embedded clinical governance. The result is a care framework designed to sustain psychiatric services over time, even as pressures on the workforce continue to evolve.
Sources:
- Archer, J., et al. (2012). Collaborative care for depression and anxiety problems. Cochrane Database of Systematic Reviews.
Firth, J., et al. (2017). The efficacy of smartphone-based mental health interventions for depressive symptoms. World Psychiatry.
Fortney, J. C., et al. (2017). A tipping point for measurement-based care. Psychiatric Services.
Kroenke, K., Spitzer, R. L., & Williams, J. B. (2001). The PHQ-9: Validity of a brief depression severity measure. Journal of General Internal Medicine.
Spitzer, R. L., Kroenke, K., Williams, J. B., & Löwe, B. (2006). A brief measure for assessing generalized anxiety disorder: The GAD-7. Archives of Internal Medicine
Written by Emily Yi
About the Authors
Emily Yi is a licensed clinical social worker who works with adolescents and families while also supporting behavioral health innovation through digital care coordination. In her role as a clinical app monitor for Precise Behavioral, she helps connect therapists, primary care providers, and psychiatric specialists to improve patient outcomes.
Editorial Contributor
This piece was edited by Greta Baker.



